Understanding Diabetic Gastroparesis
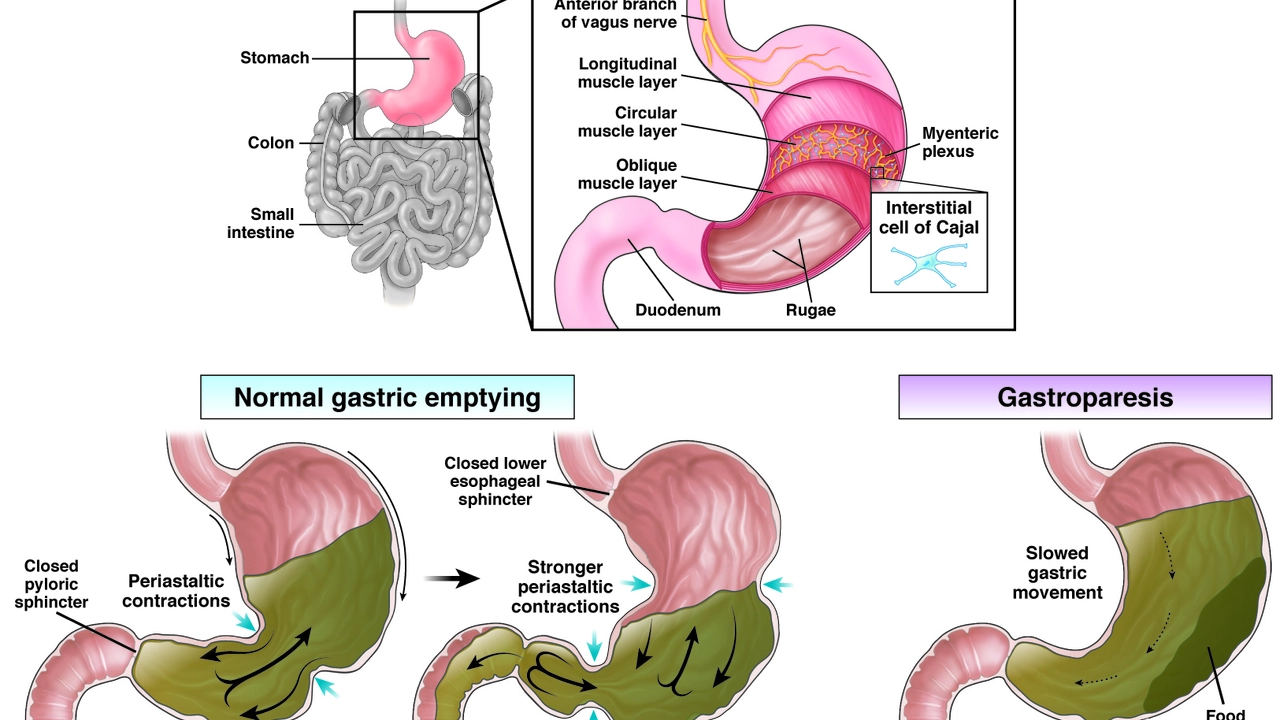
Before we delve into the role of exercise in managing diabetic gastroparesis, it's important to understand what this condition is. Gastroparesis is a condition that affects the normal movement of muscles in your stomach, often causing delayed gastric emptying. Diabetes can damage the vagus nerve, which regulates the digestive system, leading to gastroparesis. This condition can cause several symptoms like nausea, vomiting, early satiety, bloating, and abdominal pain.
The Connection Between Diabetes and Gastroparesis
Diabetes is a major risk factor for developing gastroparesis. High blood sugar levels can damage the vagus nerve over time, disrupting the movement of food through the digestive tract. This disruption can lead to the symptoms of gastroparesis. The relationship between diabetes and gastroparesis is a two-way street, as gastroparesis can also make diabetes worse by making blood sugar control more difficult.
Importance of Exercise in Diabetes Management
Exercise plays a crucial role in managing diabetes. Regular physical activity can help lower blood sugar levels, improve insulin sensitivity, and promote weight loss. It also helps in reducing stress and improving overall wellbeing. Therefore, incorporating regular exercise into your lifestyle is an effective strategy in managing diabetes and its complications, including gastroparesis.
Impact of Exercise on Gastroparesis
While the direct impact of exercise on gastroparesis is not fully understood, it has been found to aid in digestion and improve gastric emptying, thereby reducing the symptoms of gastroparesis. Regular physical activity can stimulate the muscles in the gastrointestinal tract, improving their function and coordination. This can help speed up the transit time of food through the stomach, reducing the likelihood of symptoms such as nausea, vomiting, and bloating.
Recommended Exercises for Diabetic Gastroparesis
Not all exercises are created equal when it comes to managing diabetic gastroparesis. Low-intensity activities like walking, cycling, and yoga are generally recommended. These exercises are gentle on the body and can help stimulate digestion without putting too much strain on the digestive system. High-intensity exercises, on the other hand, may not be suitable as they can divert blood flow away from the digestive system and potentially worsen symptoms.
Exercise Precautions for People with Diabetic Gastroparesis
While exercise is beneficial, it's important to take certain precautions if you have diabetic gastroparesis. It's crucial to monitor blood glucose levels before, during, and after exercise to prevent hypoglycemia. Also, make sure to stay well-hydrated and eat a small snack before exercising to provide your body with the necessary fuel. If you experience any severe symptoms like persistent nausea, vomiting, or abdominal pain, it's important to stop exercising and seek medical attention.
Role of Diet and Medication in Managing Diabetic Gastroparesis
Apart from exercise, diet and medication also play a key role in managing diabetic gastroparesis. A diet low in fat and fiber can help speed up gastric emptying and reduce symptoms. Medications like prokinetics and antiemetics may also be prescribed by your doctor to manage symptoms and improve gastric emptying. Therefore, a comprehensive approach involving exercise, diet, and medication is often the best strategy in managing diabetic gastroparesis.
Maintaining a Healthy Lifestyle with Diabetic Gastroparesis
Living with diabetic gastroparesis can be challenging, but it's certainly not impossible. Along with regular exercise, it's important to maintain a balanced diet, take prescribed medications, and monitor your blood glucose levels regularly. Regular check-ups with your healthcare provider are also crucial to monitor your condition and adjust your treatment plan as necessary. Remember, you have the power to manage your condition and maintain a healthy, active lifestyle.

Varun Gupta
July 26, 2023 AT 23:58Amy Reynal
July 27, 2023 AT 04:46Erick Horn
July 29, 2023 AT 00:17Lidia Hertel
July 30, 2023 AT 14:59Chris Bock
August 1, 2023 AT 04:00Alyson Knisel
August 1, 2023 AT 04:56Jelisa Cameron- Humphrey
August 2, 2023 AT 17:41Lee Lach
August 3, 2023 AT 04:29Tracy McKee
August 4, 2023 AT 20:36Abigail M. Bautista
August 6, 2023 AT 13:57Rohan Puri
August 7, 2023 AT 18:56Andrew Butler
August 9, 2023 AT 01:13Mandeep Singh
August 9, 2023 AT 13:34Phillip Lee
August 9, 2023 AT 23:44Nancy N.
August 10, 2023 AT 14:36Katie Wilson
August 12, 2023 AT 00:58Shivani Tipnis
August 13, 2023 AT 08:16Cindy Fitrasari S.
August 13, 2023 AT 09:25