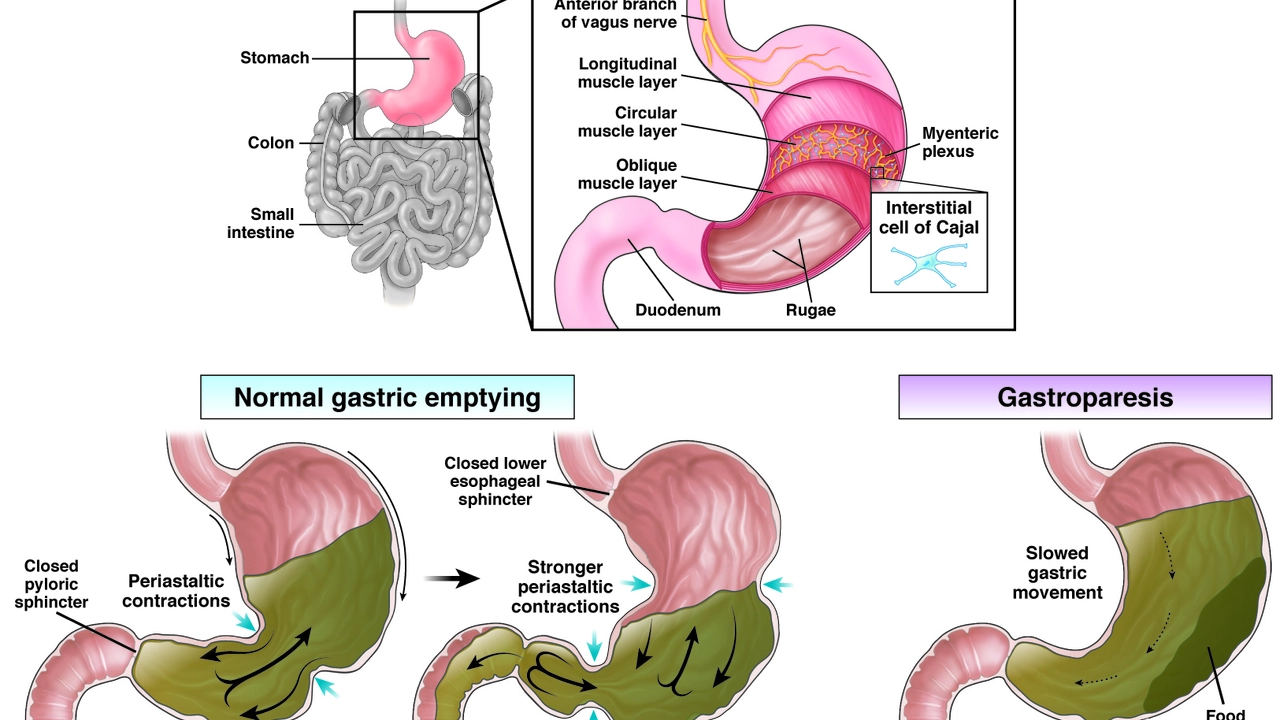
Diabetic Gastroparesis: What It Is and How to Manage It
If you have diabetes and your stomach feels like it's stuck on pause, chances are you’re dealing with gastroparesis. In plain terms, it’s a condition where the stomach empties far slower than normal because nerves that control muscle movement get damaged by high blood sugar.
Common Symptoms You Shouldn't Ignore
Typical signs include feeling full after just a few bites, nausea, occasional vomiting of undigested food, bloating, and unpredictable blood‑sugar spikes. Some people also notice weight loss without trying or erratic glucose readings that make insulin dosing a nightmare.
Practical Ways to Slow Down the Stomach Slowing
The first step is tightening blood‑sugar control. Keep your A1C as low as your doctor says is safe—steady numbers give nerves a chance to heal. Small, frequent meals work better than three big plates; aim for 5–6 mini‑meals spread through the day.
Choose foods that are easy on the stomach: lean proteins, cooked veggies, and low‑fiber fruits like bananas or canned peaches. Avoid high‑fat and very fibrous items because they sit in the gut longer and can worsen delays.
Chewing thoroughly is a simple trick many overlook. Break food down into tiny pieces before swallowing; it gives enzymes a head start and helps the stomach move stuff along more smoothly.
If you’re on insulin, consider adjusting timing based on how quickly your meals clear. Some doctors recommend taking rapid‑acting insulin right after eating rather than before, to match delayed glucose absorption.
Medications can help too. Drugs like metoclopramide or erythromycin are sometimes prescribed to boost stomach contractions. Talk with your doctor about benefits and side effects—these meds aren’t for everyone.
Staying hydrated is key, but sip fluids between meals rather than during them. Large amounts of liquid with food can further slow emptying, while regular sips keep you from getting dehydrated from vomiting or nausea.
Finally, track your symptoms in a notebook or app. Note what you eat, how you feel, and any blood‑sugar changes. Patterns emerge quickly, letting you and your doctor fine‑tune diet and meds for better control.
The Role of Exercise in Managing Diabetic Gastroparesis
In my latest exploration, I delved into the role exercise plays in managing Diabetic Gastroparesis. This often-overlooked aspect of treatment can significantly improve gastric emptying and overall gut health. Regular, moderate exercise like walking or cycling can help control blood sugar levels, which is crucial for those with this condition. It also improves digestion and reduces symptoms like bloating and nausea. So, don't underestimate the power of a good workout for managing diabetic gastroparesis!
READ MORE